Post by : Anees Nasser
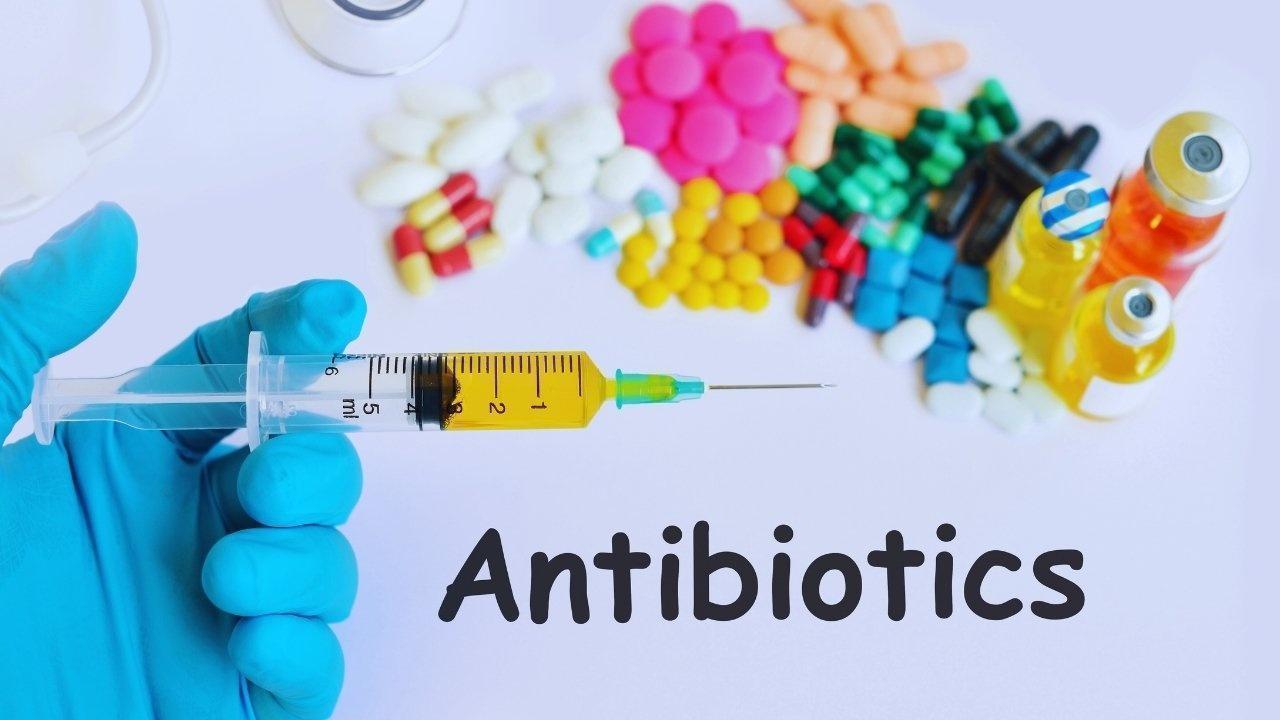
A recent overhaul of antibiotic guidelines is transforming how medical professionals prescribe treatments and how patients receive care. Released by prominent medical organizations this week, the enhancements address the pressing issue of antibiotic resistance while promoting more evidence-based prescribing practices. Though the adjustments may seem minor to patients—such as shorter treatment durations or more targeted therapeutic approaches—they signal a major shift in managing both acute and chronic infections for healthcare providers.
These updated guidelines stress the importance of using narrower-spectrum antibiotics, reducing the length of treatment, and requiring strong justification for the use of potent drugs. Following an alarming increase in antimicrobial resistance rates, attributed to past overprescribing and ineffective follow-up care, this update comes at a crucial time.
This article delves into the effects these changes will have on healthcare professionals, pharmacies, testing protocols, and long-term public health implications.
The modifications to antibiotic recommendations arise from serious global challenges.
With resistance levels rising disturbingly, typical infections are becoming progressively less treatable with standard antibiotics. Health authorities caution that these trends could escalate straightforward infections into serious health threats.
A significant number of antibiotic prescriptions are given for viral infections, where they are ineffective. The new guidelines strive to curb such unnecessary prescriptions.
Broad-spectrum antibiotics can harm beneficial bacteria, raising the likelihood of resistance. The updated recommendations favor narrower-spectrum options when appropriate.
Historically, extended treatment durations have been common, but new findings suggest that shorter courses can be just as effective.
Advances in diagnostics and microbial testing prompt the emphasis on targeted treatments rather than speculative prescribing.
This integration of scientific evidence, clinical urgency, and public-health priorities has initiated an important change to the guidelines.
For many prevalent infections—like respiratory and urinary conditions—the suggested treatment course has been shortened. Instead of 7–14 days, many cases now call for just 3–5 days, depending on severity and patient response.
Providers are encouraged to start treatment with the narrowest-spectrum antibiotic suitable for the identified pathogen.
Clinicians are advised to conduct rapid tests or symptom-based evaluations before deciding to prescribe antibiotics.
For ambiguous situations, doctors may recommend a delayed prescription, allowing patients to wait 24-48 hours before filling it, in case their symptoms resolve without antibiotics.
Medications like fluoroquinolones and advanced macrolides now require clear clinical justification for their use.
Guidelines now focus on diligent follow-up to ensure patients improve and to discontinue antibiotics if they aren’t needed.
These changes are designed to maintain antibiotic efficacy for future generations.
Patients will receive antibiotics only when necessary. Antibiotics will not be routinely prescribed for viral infections like colds or sore throats.
Patients may find that their prescribed courses are shorter than before. Clinicians assure that these shorter spans are effective and help reduce resistance.
Expect longer, more detailed questioning during visits to assess the necessity of antibiotics. This is integral for improved patient education.
Some patients will be recommended rapid tests or diagnostic procedures before receiving any antibiotic treatment.
Following test results, providers may switch patients from broad-spectrum to narrow-spectrum antibiotics.
Patients may be advised to monitor their symptoms before proceeding with a prescription.
These updates support the responsible use of antibiotics while prioritizing patient safety.
Medical professionals now emphasize diagnostics over routine prescribing, with symptom assessment tools becoming standard in clinics.
Practitioners are dedicating more time to explain when antibiotics may not be required, promoting public understanding.
Hospitals are implementing standardized infection management protocols aligned with new guidelines.
Doctors are engaging patients in conversations about their treatment options and potential outcomes.
Clinicians are required to provide clearer justifications for antibiotic prescriptions, enhancing accountability.
This results in a more structured and evidence-driven prescribing environment.
Pharmacists are essential to effective antibiotic stewardship, and the new guidelines significantly impact their responsibilities.
Pharmacists will guide patients on dosage adjustments, the importance of adherence, and understanding the significance of guideline changes.
Pharmacists will scrutinize prescriptions to ensure compliance with updated standards.
Antibiotics will not be refilled without a new prescription unless clinically justified.
Pharmacists will ensure that prescribed antibiotics do not adversely interact with patients’ chronic medications.
Pharmacies will act as frontline educators, helping patients understand what to expect during recovery and when to seek medical advice.
Patients used to receiving antibiotics may be surprised when they are advised against them.
Most patients are more accepting of the changes when their doctors explain the rationale behind them.
Patients are becoming more informed about distinguishing between viral and bacterial infections.
Shorter, targeted prescriptions are leading to fewer digestive issues, headaches, and fatigue among many patients.
There is a growing trend where individuals prioritize hydration, nutrition, and rest instead of resorting to antibiotics at the first sign of illness.
Public sentiment is gradually shifting to support responsible antibiotic usage.
Hospitals are updating procedures to enhance stewardship and monitor resistance trends more effectively.
Stricter guidelines may lead to reduced return visits prompted by antibiotic side effects.
Precision therapy minimizes the spread of drug-resistant strains within healthcare settings.
Enhanced collaboration among clinicians, pharmacists, and nurses fosters more efficient care delivery.
These modifications allow healthcare systems to allocate antibiotic resources more judiciously.
The primary goal is to curb the rise of antimicrobial resistance, a significant global health threat.
The new guidelines aim to ensure that antibiotics remain effective for severe conditions by preventing misuse.
Care guided by scientific evidence promotes long-term health outcomes for the population.
Patients are beginning to manage mild ailments without immediately resorting to antibiotics.
These adjustments resonate with global health initiatives.
Many patients still anticipate receiving antibiotics to alleviate symptoms quickly.
Explaining the new guidelines clearly requires additional time from providers during consultations.
Rapid testing may not be widely available in all regions.
In certain countries, lax regulations continue to fuel misuse of antibiotics.
Monitoring patients’ adherence to prescribed treatments presents ongoing challenges.
Despite the obstacles, progress is being achieved.
Research reveals that shorter treatment durations are effective for various infections and help mitigate resistance.
Shorter treatment periods lead to fewer cases of digestive problems and dizziness.
Patients are more inclined to complete shorter treatment courses.
Minimizing antibiotic exposure helps maintain beneficial gut bacteria, impacting long-term health positively.
This transition is reshaping treatment outcomes for the better.
Diagnostics are set to become a cornerstone in managing infections.
Portable testing devices may soon become commonplace.
Governments may increase investment in educational campaigns surrounding antibiotic use.
Tighter controls may be implemented in markets with unregulated access to antibiotics.
Clinicians may increasingly use predictive tools to inform antibiotic decisions.
This guideline revision signifies the beginning of a more intelligent and effective approach to antibiotic use.
The recent updates to antibiotic guidelines mark a significant milestone in modern healthcare. With an emphasis on shorter, more targeted treatment and enhanced diagnostic clarity, the revisions seek to mitigate the risk of antimicrobial resistance for both current and future patient populations. Although patients may encounter fewer prescriptions or shorter treatment durations, the overarching benefits will include improved care quality, reduced side effects, and strengthened public health.
As medical practices, pharmacies, and communities adapt, society makes strides towards responsible antibiotic use, ensuring these crucial medications remain potent for future generations.
This article is intended for informational and editorial purposes only, and it does not provide medical or treatment advice. Patients should consult licensed healthcare professionals regarding antibiotics or health issues.








Anticipated Dates for UAE Eid Al Adha 2026 Unveiled by Astronomical Experts
Experts predict Eid Al Adha 2026 in the UAE to start on May 27, prompting early holiday planning amo

DAE Achieves Remarkable Growth in Q1 2026 With Record Revenue
Dubai Aerospace Enterprise announces impressive financial results for Q1 2026, reflecting a surge in

Price Increase for Sony PS5 in Southeast Asia Effective May 1
Sony announces a price increase for the PS5 across Southeast Asia starting May 1, 2026, impacting ga

Potential ‘Super El Niño’ in 2026: Understanding the Climate Risks
Could a Super El Niño emerge in 2026? Discover its implications and potential global climate impacts

Global Energy Crisis Intensifies: Markets React to Oil Supply Challenges
Markets are on edge as oil disruptions escalate, influencing prices and economic stability. Explore

Must-See Tourist Spots in London You Can't Overlook
Explore London's essential attractions, from royal landmarks to vibrant markets, ensuring an unforge